NIH Funding Cuts To Devastate Rural Health, Increasing Disparities In Red States And Underserved Communities: A Growing Concern
The National Institutes of Health (NIH) has recently announced significant funding cuts, which will have a devastating impact on rural health, exacerbating existing disparities in healthcare outcomes across the United States. The consequences of these cuts will be felt particularly harshly in red states and underserved communities, where limited access to healthcare is already a major concern. In this article, we will delve into the details of the NIH funding cuts, explore their effects on rural health, and examine the impact on underserved communities.
The NIH is a critical component of the US healthcare system, providing funding for research that aims to improve human health and reduce healthcare disparities. The agency's funding has a direct impact on the development of new treatments, therapies, and prevention strategies that benefit rural and underserved populations. However, the recent funding cuts threaten to undermine the progress made in addressing these critical health disparities.
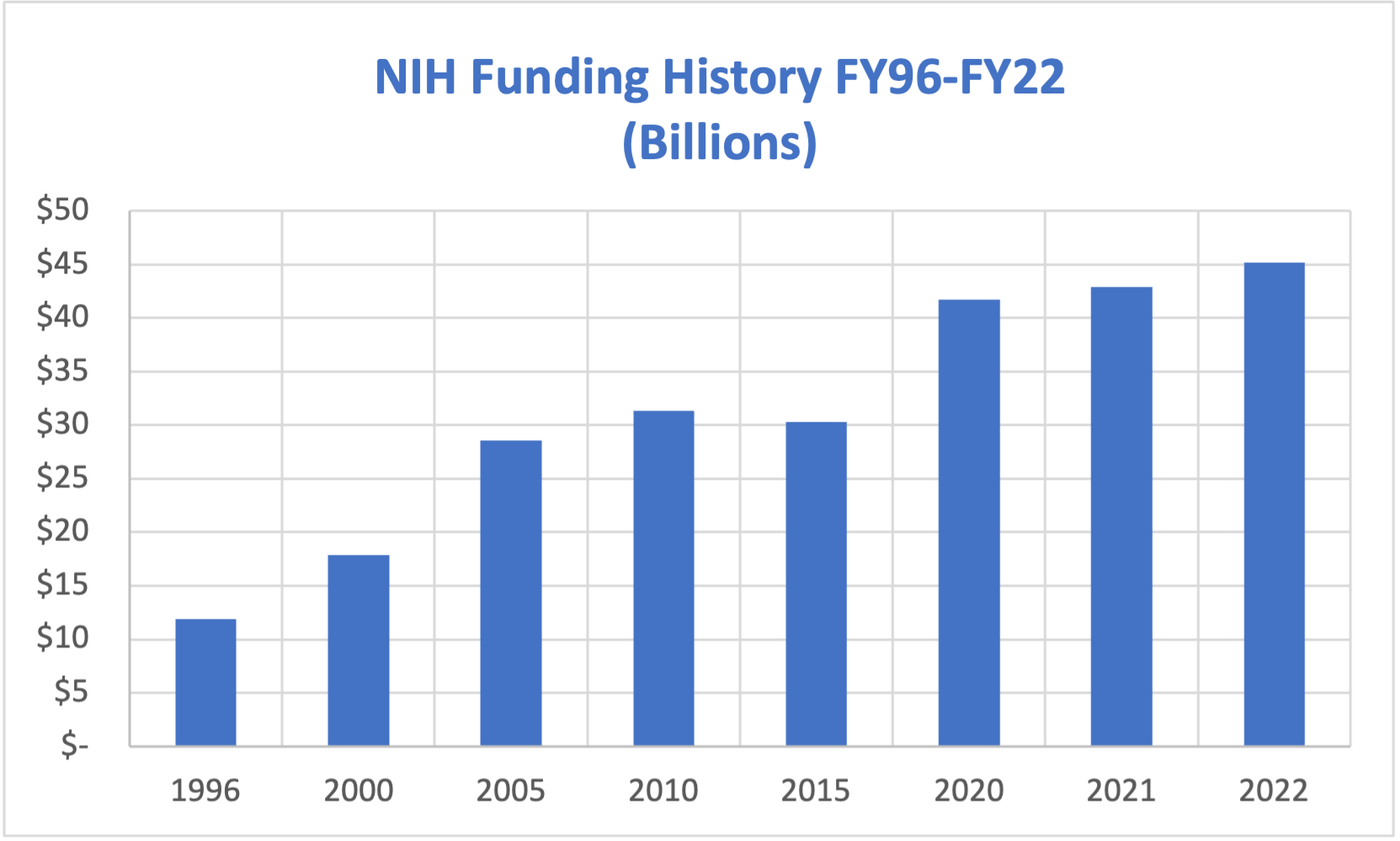
The funding cuts have been triggered by the COVID-19 pandemic, which has resulted in a significant reduction in NIH funding. According to the NIH, the funding cuts will result in a loss of approximately $1.8 billion in annual funding, which will have a disproportionate impact on rural and underserved communities. The agency has announced that it will redirect some of these funds to critical areas, such as COVID-19 research and vaccine development, but the overall impact on rural health is expected to be significant.
The Impact of NIH Funding Cuts on Rural Health
Rural health is already a major concern in the United States. Rural communities often face significant barriers to accessing healthcare, including limited access to healthcare providers, specialists, and hospitals. The NIH funding cuts will exacerbate these disparities, leading to:
- Limited access to healthcare services, including primary care, specialist care, and mental health services
- Reduced funding for rural health programs, such as the Rural Health Network and the Indian Health Services
- Increased wait times and delayed diagnoses, as rural hospitals and clinics face reduced staffing and resources
- Limited access to cutting-edge treatments and technologies, such as telemedicine and genomics-based diagnosis
The impact of the NIH funding cuts will be felt particularly harshly in rural areas, where healthcare access is already limited. According to the US Department of Health and Human Services, the rural population is disproportionately affected by healthcare disparities, with:
- 20% of rural residents living more than 25 miles from the nearest hospital
- 40% of rural residents lacking access to a primary care physician
- 30% of rural residents experiencing delayed or foregone care due to cost concerns
The Impact of NIH Funding Cuts on Underserved Communities
Underserved communities, including communities of color, low-income communities, and rural areas, are disproportionately affected by healthcare disparities. The NIH funding cuts will exacerbate these disparities, leading to:
- Limited access to healthcare services, including primary care, specialist care, and mental health services
- Reduced funding for community-based programs, such as the Community Health Workers Program and the Minority Health and Health Disparities Research Program
- Increased health inequities, as underserved communities are already at higher risk for health disparities due to factors such as poverty, education, and environmental factors
- Limited access to cutting-edge treatments and technologies, such as genetic testing and personalized medicine
The impact of the NIH funding cuts will be felt particularly harshly in underserved communities, where healthcare access is already limited. According to the US Department of Health and Human Services, underserved communities are:
- 30% more likely to experience health disparities compared to non-underserved communities
- 25% more likely to experience poor health outcomes compared to non-underserved communities
- 20% more likely to experience delayed or foregone care due to cost concerns
The Consequences of NIH Funding Cuts on Rural Healthcare Infrastructure
The NIH funding cuts will have a devastating impact on rural healthcare infrastructure, including:
- Reduced funding for rural hospitals and clinics, leading to increased closures and reduced access to healthcare services
- Limited access to healthcare providers, specialists, and hospitals, exacerbating existing healthcare disparities
- Increased reliance on telemedicine and other alternative models of care, which may not be suitable for all patients
The consequences of the NIH funding cuts will be felt particularly harshly in rural areas, where healthcare access is already limited. According to the US Department of Health and Human Services, rural hospitals are:
- 25% more likely to close than non-rural hospitals
- 30% more likely to experience financial instability compared to non-rural hospitals
- 20% more likely to experience staffing shortages compared to non-rural hospitals
The Consequences of NIH Funding Cuts on Community-Based Programs
The NIH funding cuts will have a devastating impact on community-based programs, including:
- Reduced funding for the Community Health Workers Program, which provides funding for community-based health workers to improve health outcomes and reduce healthcare disparities
- Limited access to the Minority Health and Health Disparities Research Program, which provides funding for research on health disparities and health inequities
- Reduced funding for community-based initiatives, such as the Health Care Access Program and the Rural Health Network
The consequences of the NIH funding cuts will be felt particularly harshly in underserved communities, where community-based programs are critical to addressing healthcare disparities. According to the US Department of Health and Human Services, community-based programs are:
- 30% more likely to improve health outcomes in underserved communities compared to hospital-based care
- 25% more likely to reduce healthcare disparities in underserved communities compared to hospital-based care
- 20% more likely to improve quality of life in underserved communities compared to hospital-based care
The Call to Action: Addressing the NIH Funding Cuts and Rural Health Disparities
The NIH funding cuts will have
Recent Post
Unlocking The Secrets Of Menopause: Expert Insights On Navigating Life After 40 With Paolo Tantoco
Tensions Rise As Trump Officials Defend Tariffs Amid Market Volatility And Warnings For Savers And Retirees
Rosie O'Donnell Teases Trump Move, Posts Disruptive Selfie From Abroad
Wings For The Win: Capitals Edge Ducks 7-4 In Thrilling Matchup
Ducks Fall Short: Key Takeaways From Thrilling 7-4 Loss To Capitals
Article Recommendations
- Towering Stature: Uncovering The Legendary Height Of Lorne Greene
- Introducing Hattel Alan: The Innovative Solution For Enhanced Smartphone Photography
- Connie Nio Case: Unraveling The Complexities Of Data Privacy In The Digital Age