Unveiling the Hidden Threat: Bacterial Vaginosis A Hidden STI Waiting To Be Treated
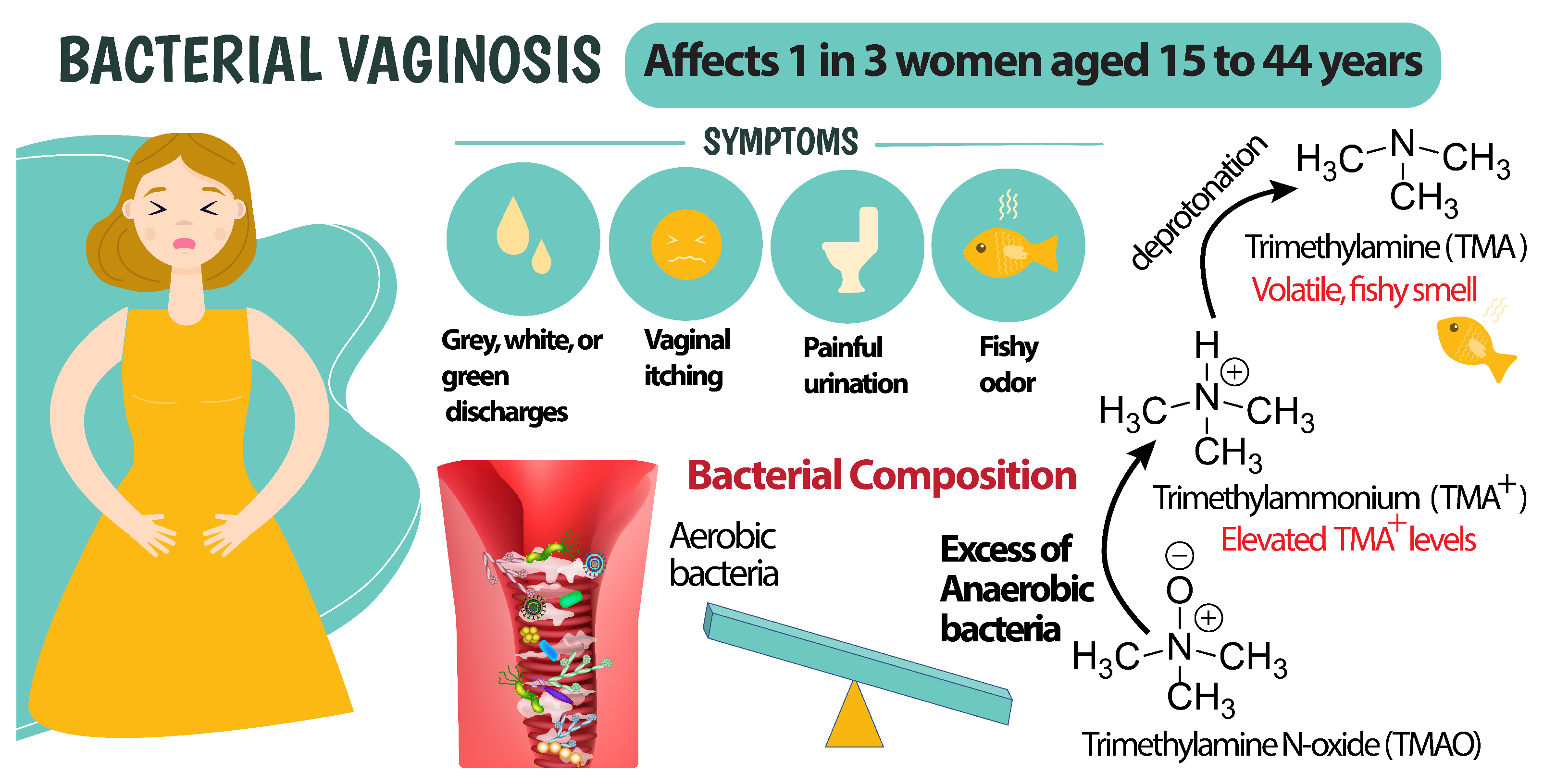
Bacterial vaginosis, often referred to as BV, is a sexually transmitted infection (STI) that affects millions of women worldwide. Despite its prevalence, BV remains a hidden threat, often misdiagnosed or undertreated due to its subtle symptoms and lack of awareness. However, this STI is not a trivial issue and requires attention from healthcare providers and the general public alike.
The prevalence of BV varies depending on factors such as age, reproductive history, and geographical location. According to the Centers for Disease Control and Prevention (CDC), approximately 29% of women of reproductive age in the United States have BV. Furthermore, BV is more common among women who are:
• Under 25 years old
• Having multiple sex partners
• Not using condoms consistently
• Having a history of pelvic inflammatory disease (PID)
• Having a history of STIs
The symptoms of BV can be mild, and some women may not experience any noticeable symptoms at all. However, when symptoms do occur, they may include:
• Thin, white, or yellowish discharge with a strong fishy odor
• Burning sensation while urinating
• Abdominal pain or cramping
• Fever
• Redness and irritation of the vulva
The exact cause of BV is not fully understood, but it is believed to be a result of an imbalance of the natural bacterial flora in the vagina. A healthy vaginal microbiome is typically composed of lactobacilli, which help to maintain the vagina's acidity and prevent the growth of harmful bacteria. In women with BV, the presence of anaerobic bacteria, such as Gardnerella vaginalis, disrupts this balance, leading to an overgrowth of these bacteria.
Types of Bacterial Vaginosis
While BV is often referred to as a single entity, there are several subtypes of the condition, each with distinct characteristics. These subtypes include:
Normal and Imbalanced Vaginal Flora
Normal vaginal flora is composed of a diverse range of microorganisms, including lactobacilli, which help to maintain the vagina's acidity. In women with BV, the presence of anaerobic bacteria disrupts this balance, leading to an overgrowth of these bacteria.
Characteristics of Normal Vaginal Flora
• Lactobacilli
• Bifidobacterium
• Streptococcus
• Enterococcus
Characteristics of Imbalanced Vaginal Flora in BV
• Overgrowth of anaerobic bacteria, such as Gardnerella vaginalis
• Decreased presence of lactobacilli
• Presence of other pathogenic bacteria, such as Escherichia coli (E. coli) and Klebsiella pneumoniae
Amebiasis and Trichomoniasis
In some cases, BV may be caused by other STIs, such as amebiasis or trichomoniasis. These conditions can lead to similar symptoms, making diagnosis more challenging.
Characteristics of Amebiasis
• Presence of Entamoeba histolytica in the vaginal discharge
• Characterized by a thin, watery discharge with a strong, fishy odor
• May be accompanied by abdominal pain and rectal bleeding
Characteristics of Trichomoniasis
• Presence of Trichomonas vaginalis in the vaginal discharge
• Characterized by a frothy, yellowish discharge with a strong, unpleasant odor
• May be accompanied by burning sensation while urinating and abdominal pain
Diagnosis and Testing
Diagnosing BV can be challenging, as the symptoms are often non-specific and may be similar to those of other STIs. A healthcare provider may use a combination of clinical evaluation, medical history, and laboratory tests to diagnose BV.
Clinical Evaluation
A healthcare provider may perform a pelvic exam to evaluate the vulva, vagina, and cervix for signs of inflammation or infection. They may also ask about symptoms, medical history, and reproductive history.
Laboratory Tests
Several laboratory tests can help confirm the diagnosis of BV, including:
Nucleic Acid Amplification Tests (NAATs)
• Highly sensitive and specific for detecting BV
• Can detect the presence of anaerobic bacteria, such as Gardnerella vaginalis
• May be performed on a vaginal swab or discharge sample
Gram Stain Tests
• Can detect the presence of anaerobic bacteria, such as Gardnerella vaginalis
• May be performed on a vaginal swab or discharge sample
• Less sensitive and specific than NAATs
Treatment and Management
Treatment for BV typically involves antibiotics, which can help restore the natural balance of the vaginal microbiome and reduce symptoms. In some cases, antifungal or antibacterial creams may be prescribed to treat co-infections.
Antibiotic Treatment
Antibiotic treatment for BV typically involves a course of metronidazole or clindamycin. These antibiotics can help reduce symptoms and prevent complications.
Metronidazole
• Effective in treating BV
• May be prescribed in combination with an antiprogestin hormone
• May be taken orally or intravaginally
Clindamycin
• Effective in treating BV
• May be prescribed in combination with an antiprogestin hormone
• May be taken orally or intravaginally
Management of Symptoms
In addition to antibiotic treatment, there are several ways to manage symptoms of BV, including:
Practice Good Hygiene
• Wear loose, breathable clothing
• Avoid scented soaps, douching, and fragrances
• Wipe from front to back to prevent bacterial transfer
Use Moisture-Repellent Products
• Use vaginal moisturizers or lubricants to reduce dryness and irritation
Recent Post
Unlocking The Secrets Of Menopause: Expert Insights On Navigating Life After 40 With Paolo Tantoco
Tensions Rise As Trump Officials Defend Tariffs Amid Market Volatility And Warnings For Savers And Retirees
Rosie O'Donnell Teases Trump Move, Posts Disruptive Selfie From Abroad
Wings For The Win: Capitals Edge Ducks 7-4 In Thrilling Matchup
Ducks Fall Short: Key Takeaways From Thrilling 7-4 Loss To Capitals
Article Recommendations
- Meet Janice Nichole Rivera: Social Media Marketing Trailblazer And Thought Leader
- Unveiling Sabrina Carpenter's Stature: Inside The Actress-Singer's Height
- Unraveling The Karlan And Connieenio Crime Saga: A Shocking Tale Of Betrayal And Deceit